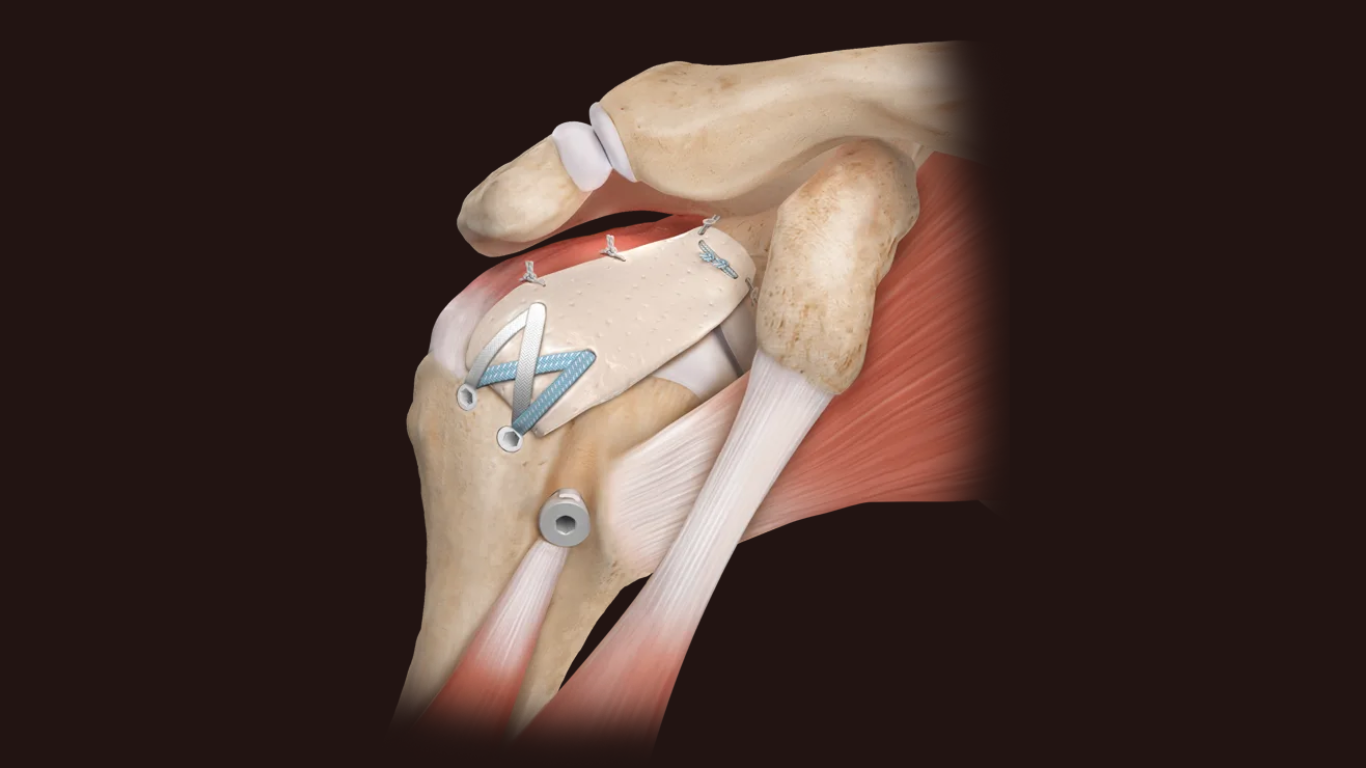
Massive irreparable rotator cuff tears (MIRCTs) in the posterosuperior shoulder remain one of the more humbling problems in sports medicine. The tendon is gone. The muscle is fatty. The humeral head is migrating north. And the patient — often in their early 60s — is not thrilled about the words “reverse shoulder arthroplasty.”
That’s where superior capsular reconstruction (SCR) continues to hold interest.
A recent Level IV study evaluated arthroscopic SCR using a human-derived acellular collagen matrix (hACM) in patients with posterosuperior MIRCTs, with a minimum two-year follow-up.
The question: does a biologic, non-prosthetic reconstruction provide meaningful and durable improvement?
The Shoulder in Question
Between 2018 and 2021, investigators retrospectively reviewed 48 patients who underwent arthroscopic SCR with hACM.
Inclusion criteria were pragmatic and familiar: intact or repairable subscapularis, failed nonoperative care, age under 80, Goutallier ≤2 for infraspinatus and minimum two-year follow-up.
The primary outcome was the Constant–Murley score (CMS). Radiographically, the authors assessed acromiohumeral interval (AHI) and graft integrity at two years.
Mean age? 63.5 years. Follow-up? About 26 months.
In other words: the classic “too young for reverse, too symptomatic to ignore” cohort.
The Numbers That Matter
Preoperatively, median Constant–Murley score was 39.5. At one year post-op, that jumped to 73. At two years, it reached 76.
The improvements were statistically significant (p < 0.0001) and, more importantly, clinically meaningful.
Only two patients (4.2%) failed to reach the minimal clinically important difference at two years.
Pain improved. ADLs improved. Range of motion improved. Strength improved.
For surgeons counseling these patients, that’s not trivial. That’s a functional shoulder.
But What About the Graft?
Here’s where things get interesting.
At two years, graft integrity was present in 41.7% of cases. Less than half of grafts were radiographically intact. And yet, clinical outcomes did not significantly differ between patients with and without graft integration.
That finding echoes what many shoulder surgeons have suspected: Superior capsular reconstruction may function less as a permanent structural spacer and more as a biologic and biomechanical reset.
However, radiographs did tell part of the story. Mean preoperative acromiohumeral interval (AHI) was 0.58 cm. Postoperatively, it measured 0.51 cm (p = 0.031).
When broken down by integration: In patients with graft integration, AHI remained stable. In those without integration, AHI decreased significantly.
So graft healing did appear to influence humeral head position — even if it didn’t clearly separate clinical outcomes at two years.
What This Means in the Real World
SCR continues to occupy a middle lane between debridement and reverse arthroplasty.
This study suggests that using human acellular collagen matrix:
- Produces meaningful functional gains at two years
- Carries a low rate of patients failing to reach MCID
- Shows modest graft integration rates
- May help stabilize superior migration when integration occurs
Importantly, this is a case series with no comparison group. It does not settle the autograft vs. allograft debate. It does not answer durability beyond two years. And it does not establish superiority over other options.
But it does reinforce something many surgeons are navigating daily: For the 60-something patient with an irreparable posterosuperior tear who still wants to remain active — and avoid a prosthesis — SCR remains a viable tool in the armamentarium.
Even if the graft doesn’t always look perfect on MRI. Sometimes, the shoulder just needs a biologic assist long enough to restore function. And sometimes, that’s enough.
Origin Study Title Link: Superior capsular reconstruction using human acellular collagen matrix: A 2-year follow-up study in posterosuperior massive irreparable rotator cuff tears
Authors: Pablo Terol-Alcayde, Víctor Martín-Gorgojo, Emilio Ferrando-Meseguer, Antonio Silvestre-Muñoz