Sometimes the smallest joint in the hand can cause some of the biggest problems.
Thumb carpometacarpal (CMC) osteoarthritis is one of those conditions that quietly erodes quality of life, making everyday tasks like opening jars, turning keys, or gripping tools surprisingly painful.
Now, a team at Tampa General Hospital (TGH) and Florida Orthopaedic Institute is bringing a new option to the surgical toolbox. The institutions recently performed Florida’s first procedures using the TOUCH® CMC prosthesis, a new artificial joint designed by Keri Medical SA specifically to treat advanced thumb CMC arthritis.
The surgery was performed by orthopedic surgeons Devin Collins, M.D. and Alfred Hess, M.D., marking the state’s debut of the implant and placing the Tampa-based program among a small group of early adopters nationwide.
Thumb CMC arthritis is extremely common, particularly in older adults and patients whose work or hobbies demand repetitive pinch and grip. While conservative care — splinting, non-steroidal anti-inflammatory drugs, steroid injections and therapy — can provide relief, many patients eventually reach the point where surgery becomes the next step.
Traditionally, the gold standard surgical intervention has been trapeziectomy with ligament reconstruction and tendon interposition. The procedure works well for pain relief, but it does rely on removal of the trapezium and the body’s ability to create a fibrous cushion over time. That approach can sometimes come with trade-offs such as loss of thumb height, pinch strength changes, or prolonged rehabilitation.
The TOUCH CMC Prosthesis Alternative
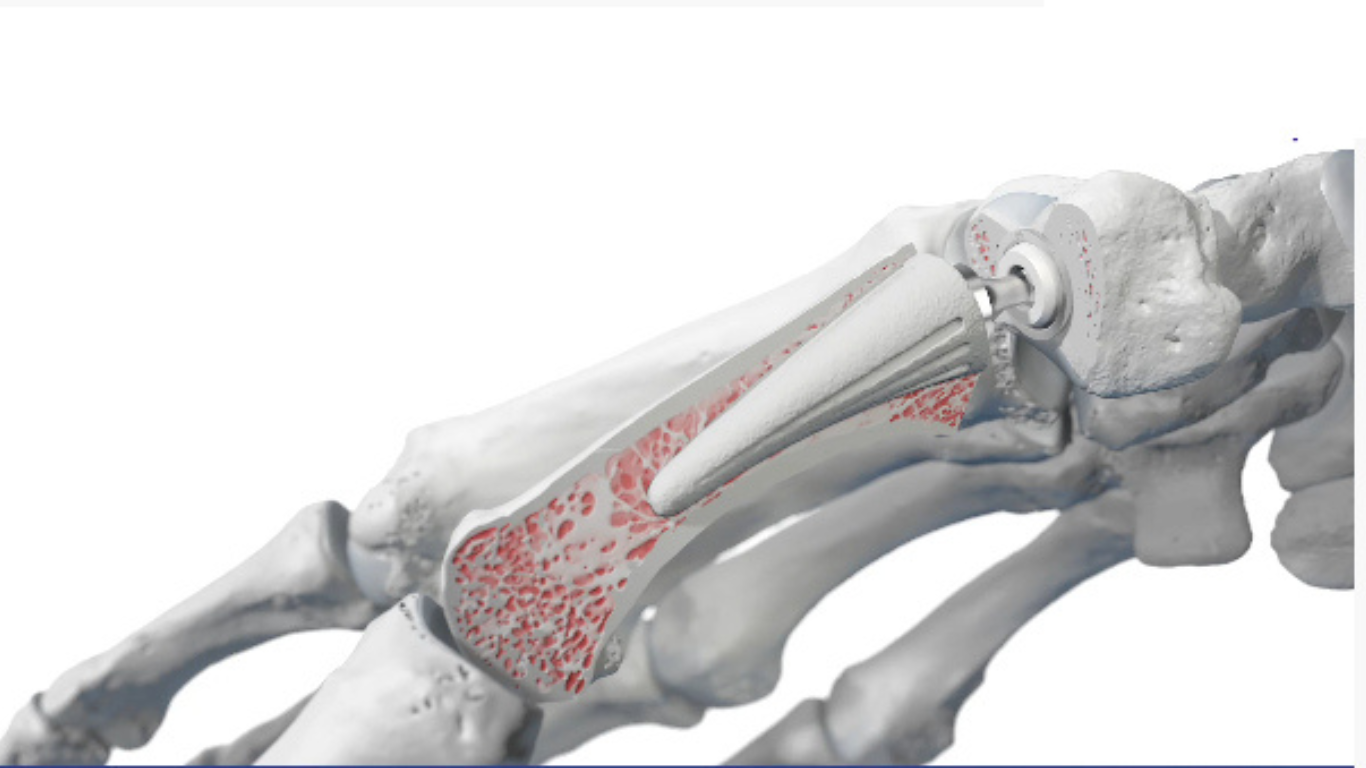
The TOUCH CMC prosthesis is the first implant in the United States to receive FDA approval for total joint replacement of the first CMC joint. Instead of removing bone and relying on soft tissue to fill the gap, the device replaces the arthritic joint with a dual-mobility ball-and-socket design intended to mimic natural biomechanics.
The goal is straightforward: preserve thumb length, restore stability, and give patients stronger, more natural movement.
For surgeons, the concept may feel familiar. Total joint arthroplasty transformed hip and knee care decades ago. Bringing a similar philosophy to the thumb represents a fascinating evolution in hand surgery.
According to Roy Sanders, M.D., chief of the TGH Orthopaedic Institute and president and chief medical officer of the Florida Orthopaedic Institute, the procedure reflects a broader commitment to innovation and evidence-based care.
The implant is currently in limited market release and has been introduced in about 20 facilities across the United States. Florida Orthopaedic Institute was selected as one of the early launch sites, in part due to its national reputation and longstanding fellowship program that trains the next generation of orthopedic surgeons.
For Dr. Hess, the moment represents more than just the introduction of a new device. It signals a shift toward expanding options for patients who want to maintain strength, dexterity, and independence.
Similarly, Dr. Collins sees the prosthesis as part of a larger trend in musculoskeletal care: moving beyond pain relief alone and focusing on restoring full function.
If the implant delivers on its early promise, it could reshape how surgeons think about treating moderate to severe thumb CMC arthritis. For patients who depend on their hands every day — from mechanics and craftsmen to grandparents opening snack bags for toddlers — that small joint may soon have a much bigger solution.
And for orthopedic surgeons watching the evolution of hand arthroplasty, it’s another reminder that innovation doesn’t always come in large packages. Sometimes it fits right at the base of the thumb.