Hip instability. Despite an elegant surgical approach, perfect cup positioning, meticulous soft tissues balancing, dislocation remains a frustrating, humbling complication after total hip arthroplasty (THA).
Over the years, one strategy has been simple: go bigger.
Larger articulations increase jump distance, improve impingement-free range of motion, and theoretically reduce the likelihood of the femoral head escaping the acetabular socket.
Two modern ways of achieving this stability boost have taken center stage: dual mobility (DM) constructs and jumbo heads (JH) — typically defined as femoral heads ≥ 40 mm.
Both approaches promise stability. Both have supporters. And both come with unique tradeoffs. A recent large registry-based cohort study set out to answer the question: When it comes to stability after primary THA, is dual mobility actually better than simply using a really big head?
Let’s take a look.
The Study: A Registry Battle of Big Articulations
Using a large United States joint registry, investigators analyzed 9,532 primary THAs performed between 2010 and 2024.
The breakdown: 1,716 dual mobility hips and 7,816 jumbo head hips (≥40 mm)
To keep the comparison fair, the authors only included acetabular components that could accept either articulation option. That clever design helps control for one of the biggest confounders in registry research — implant compatibility and surgeon selection bias.
The Headline Result: Pretty Similar Dislocation Rates
At six years: dual mobility dislocation rate: 2.4% and jumbo head dislocation rate: 2.2%
Despite different implant mechanics and theoretical advantages, the overall dislocation rates were remarkably similar.
But the story gets more interesting when you look at timing.
Early Advantage: Dual Mobility Wins the First Round
During the early postoperative period, dual mobility had a clear edge. Before 4.25 years, DM implants showed: 48% lower dislocation risk (Hazard ratio: 0.52)
Why might that be?
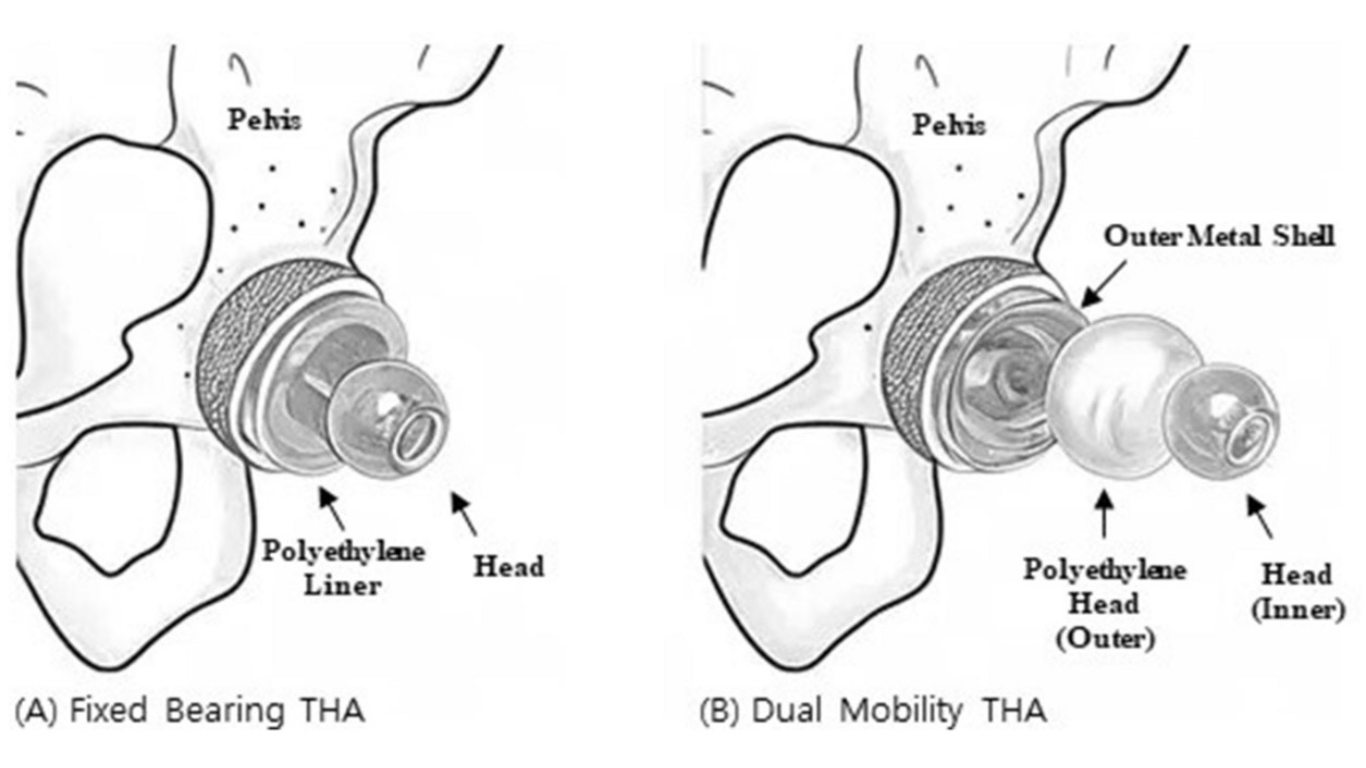
Dual mobility designs essentially create two articulations: small femoral head inside a polyethylene liner and large polyethylene liner articulating with the acetabular shell. This design increases effective head size, jump distance and arc of motion before impingement.
Biomechanically, it behaves like an enormous head without the volumetric wear concerns of a massive metal articulation. In the early years after surgery — when soft tissues are still adapting and patient activity patterns are evolving — that extra stability may matter.
The Late Twist: Jumbo Heads Come Back
But here’s the twist that makes this study particularly interesting. After 4.25 years, the trend flipped. Late dislocation risk appeared higher in the dual mobility group. The hazard ratio jumped to 8.26.
Before anyone panics, two important caveats: the absolute number of late dislocations was small and the long-term follow-up in this window was limited.
Still, the finding raises intriguing questions. While modern dual mobility designs have dramatically reduced classic intraprosthetic dislocation rates, the mechanics remain inherently more complex than a standard large-head construct.
What about revisions?
Here’s where things level out again. Despite the early and late dislocation trends, the study found no meaningful difference in revision rates between the two groups.
A Subtle but Interesting Clinical Detail
One nuance in the data deserves attention. When jumbo heads dislocated early, they were usually treated successfully with closed reduction. But when dual mobility hips dislocated, they were more likely to require revision.
Why?
Because dual mobility dislocations can sometimes represent intraprosthetic dislocation, liner disengagement and/or component-related instability.
These scenarios are harder to fix with a simple reduction. So, while DM may prevent some early dislocations, the few that occur may be more complex.
The Bottom Line
Dual mobility and jumbo heads both represent powerful tools in the quest to prevent hip instability.
This large registry study suggests that dual mobility may reduce early dislocation risk, jumbo heads perform just as well overall and revision rates are essentially the same.
Sometimes the debate isn’t about which implant is better. It’s about which one is best for the patient in front of you.
Origin Study Title: Dual Mobility Versus Jumbo Head (≥ 40 mm) Following Primary Total Hip Arthroplasty: A Registry-Based Cohort Study
Authors: Foster Chen, M.D.; Heather A. Prentice, Ph.D.; Brian H. Fasig, Ph.D.; Elizabeth W. Paxton, Ph.D.; Monti Khatod, M.D.; Kanu Okike, M.D. MPH