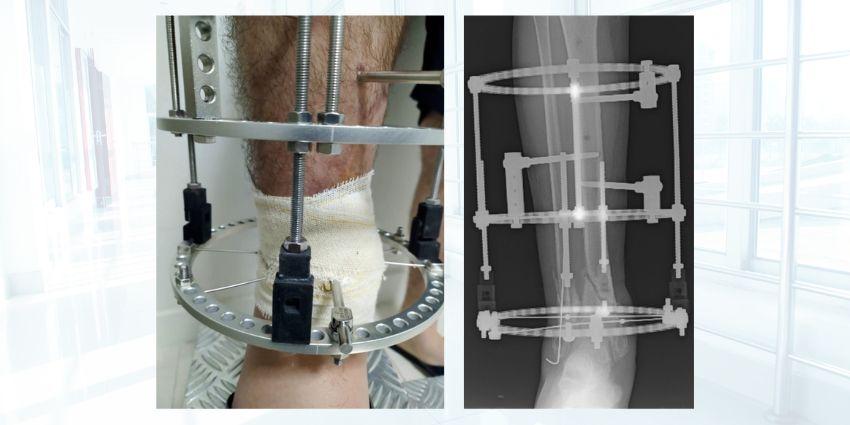
Every trauma surgeon knows the love–hate relationship with circular external fixators. They’re unmatched for segmental defects, infected tibias, mangled soft tissue — but they ask a price: long frame times, cranky pin sites, and the maddening stall of callus that just won’t bridge.
A team out of Curitiba, Brazil, may have found a clever workaround. In a double-blinded randomized clinical trial (RCT) published in the European Journal of Trauma and Emergency Surgery (September 3, 2025), “Novel device for controlled dynamization of tibial fractures: randomized clinical trial,” Fernando Ferraz Faria, Jamil Faissal Soni, Rodrigo Nunes Rached, and Paula Cristina Trevilatto tested whether controlled dynamization could coax tibias toward earlier union.
The Trial, in Brief
- 43 adults randomized to standard circular fixation vs. fixation plus a 3D-printed dynamization module
- The add-on was clipped onto frames 60 days after surgery, left for 30 days, then removed
- Monthly follow-up for up to 8 months, with blinded radiographic reads
The Punchline
- Non-union was significantly more common in the control arm (p = 0.027)
- Mean consolidation time: ~4.5 months with dynamization vs. ~6 months with standard care
- Complications: 5.2% with dynamization vs. 16.6% without
That’s a 30-day gain in healing and a threefold drop in setbacks — with nothing more exotic than measured axial micromotion at just the right time.
Why Surgeons Should Care
We’ve all been taught that bone biology loves a bit of strain — too little and it stalls, too much and it shatters. External fixators, with their “iron-bar” stiffness, often overshoot to the protective side. This Brazilian device operationalizes long-standing theory: let the frame stay rock-solid early, then loosen the leash just enough once biology is primed.
Practical Pearls for Clinic
- When: Around 2 months post-fixation — an easy calendar mark
- How long: About 30 days, finite and manageable
- Imaging: No CT or advanced studies needed, just standard X-rays
- Upside: Shorter frame times, fewer complications, happier patients (and happier trauma teams)
Caveats: It’s a single-center study with just 43 patients, so enthusiasm should be tempered until larger, multi-site trials weigh in. Still, the concept is pragmatic, reproducible, and rooted in principles that every AO course has hammered home for decades: biology likes to share the load.
The Bottom Line
For surgeons still wrestling with stubborn tibias in circular frames, controlled late dynamization could be the next incremental trick — simple, mechanical, and patient-friendly. It’s not a moonshot, but maybe that’s the point. Sometimes, getting bone to heal just takes a nudge in the right direction.